Choose risk-first compliance that’s always on, built for you.
Go back to blogs
HIPAA Covered Entities vs. Non-Covered Entities: Everything You Need to Know
Last updated on
May 26, 2025
min. read

The Health Insurance Portability and Accountability Act (HIPAA) is a landmark piece of legislation enacted in 1996 to safeguard the privacy and security of individuals’ health information.
As the healthcare arena has evolved, so has the need for regulations protecting patient data in an increasingly digital world. Understanding HIPAA is crucial for healthcare providers, insurers, and other entities managing health information.
One of the most important aspects of HIPAA is the classification of covered entities—organizations that are required to comply with its provisions. Grasping who qualifies as a covered entity is vital for ensuring compliance and maintaining patient trust in the healthcare system.
What is HIPAA?
HIPAA is designed to improve the efficiency of the healthcare system while protecting patient information from unauthorized access and disclosure. Its primary purpose is to ensure that individuals’ medical records and other personal health information are kept private and secure.
Key provisions of HIPAA focus on:
These provisions not only empower patients by granting them control over their health data but also impose strict guidelines on how healthcare entities handle sensitive information.
Also read: Guardians of healthcare data: Mastering HIPAA audit trail requirements
HIPAA’s role in protecting patient privacy
HIPAA plays a crucial role in protecting patient information by establishing strict regulations around the use and disclosure of protected health information (PHI).
The Act mandates that covered entities implement appropriate safeguards, both administrative and technical, to ensure that sensitive health data is secure from unauthorized access.
Key provisions include the right of patients to:
- Access their health records
- Request corrections
- Receive notifications in the event of a data breach.
These protections not only help maintain the confidentiality of patient information but also empower individuals by giving them control over their own health data.
Also read: How to map HIPAA to ISO 27001?
Impact of HIPAA on patient trust and healthcare practices
The implementation of HIPAA has significantly enhanced patient trust in the healthcare system.
When patients know their health information is protected, they are more likely to share sensitive details with their healthcare providers, which is vital for accurate diagnoses and effective treatment.
This trust fosters better patient-provider relationships and encourages open communication, ultimately improving the quality of care.
Additionally, HIPAA has influenced healthcare practices by promoting standardized processes for handling patient information, which helps reduce errors and enhances efficiency in care delivery.
Also read: GDPR vs HIPAA compliance: What’s the difference?

Who enforces HIPAA?
HIPAA is enforced by several government agencies in the United States, each with its own specific responsibilities related to HIPAA compliance.
The main entities responsible for enforcing different aspects of HIPAA are:
A. Office for Civil Rights (OCR)
The OCR, a part of the U.S. Department of Health and Human Services (HHS), is the primary enforcer of HIPAA. Its main role is to oversee and enforce the Privacy Rule and the Security Rule, which pertain to the privacy and security of protected health information (PHI). The OCR investigates complaints, conducts audits, and provides guidance to covered entities and business associates to ensure compliance with these rules.
B. Centers for Medicare & Medicaid Services (CMS)
CMS is responsible for enforcing the Administrative Simplification provisions of HIPAA, which include the transaction standards, code sets, and unique identifiers. CMS ensures that covered entities use standardized electronic transactions when dealing with healthcare information for billing and other purposes.
C. Department of Justice (DOJ)
The DOJ may become involved in HIPAA enforcement in cases where willful criminal violations of HIPAA occur, such as healthcare fraud, identity theft, or intentional unauthorized disclosure of PHI. The DOJ can prosecute individuals and entities for criminal violations of HIPAA.
D. State Attorneys General
State Attorneys General also have a role in enforcing HIPAA, particularly with regard to state laws that are more stringent than federal HIPAA regulations. They can investigate and take legal action against entities for HIPAA violations that affect residents in their respective states.
E. HHS Office of Inspector General (OIG)
The OIG investigates cases of healthcare fraud and abuse, which may include violations of HIPAA. While the OIG primarily focuses on financial misconduct, it may collaborate with other agencies, such as the OCR or DOJ, when investigating HIPAA-related matters.

Also read: Who enforces HIPAA?
Covered entities under HIPAA
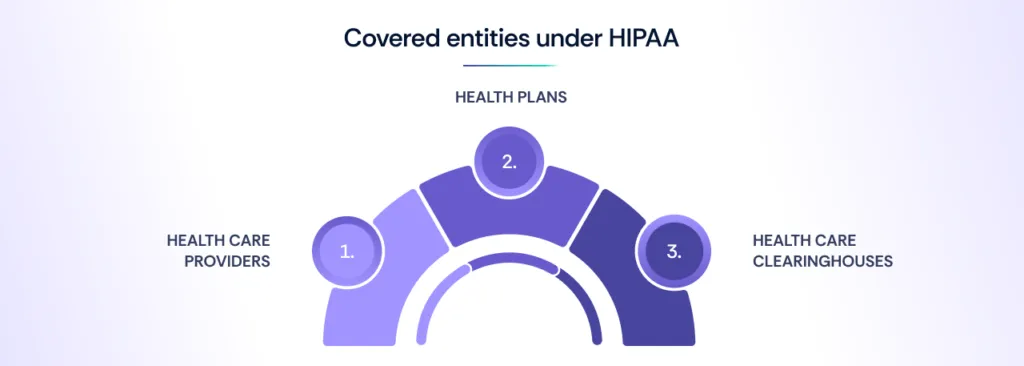
Covered entities are defined as organizations or individuals that must comply with HIPAA regulations. This designation includes those who create, receive, maintain, or transmit protected health information (PHI) in electronic form.

Health care providers
Health care providers include hospitals, physicians, dentists, and other professionals who provide medical services. To be considered a covered entity, these providers must engage in electronic health transactions, such as billing or claims processing. By doing so, they are obligated to adhere to HIPAA’s privacy and security requirements.
Health plans
Health plans consist of organizations like insurance companies, health maintenance organizations (HMOs), and government programs (such as Medicare and Medicaid). Their primary responsibilities under HIPAA involve safeguarding PHI and ensuring that patient information is handled in compliance with regulatory standards.
Health care clearinghouses
Healthcare clearinghouses are entities that process health information received from other covered entities, often converting it into standardized formats. They play a critical role in the healthcare system by facilitating the exchange of information and ensuring that data is accurately transmitted between providers and payers.
Examples include billing services and electronic data interchange (EDI) companies, which are essential for the smooth functioning of healthcare transactions.
Understanding these categories is essential for compliance with HIPAA regulations and for promoting a secure and trustworthy environment for managing health information.
Also read: What is the difference between SOC 2 vs HIPAA compliance?
Role of business associates
Business associates are individuals or entities that perform services on behalf of a covered entity that involve the use or disclosure of protected health information (PHI).
They play a vital role in the healthcare ecosystem by providing essential services, such as data processing, billing, or legal consulting.
Because they have access to sensitive health information, ensuring that business associates comply with HIPAA is critical for protecting patient privacy and maintaining trust in the healthcare system.

HIPAA business associates have specific responsibilities and obligations under HIPAA:
- Business associate agreements (BAAs): They must enter into BAAs with HIPAA-covered entities before handling PHI. These agreements outline the terms and conditions for safeguarding PHI and complying with HIPAA regulations.
- Security safeguards: HIPAA business associates are required to implement appropriate administrative, physical, and technical safeguards to protect PHI. This includes measures to prevent unauthorized access, disclosure, and breaches.
- HIPAA training: Employees of HIPAA business associates should receive training on HIPAA regulations to ensure they understand their responsibilities and the importance of PHI protection.
- Incident reporting: HIPAA business associates must report any breaches or security incidents involving PHI to the covered entity promptly.
- Subcontractor compliance: If HIPAA business associates use subcontractors (sub-business associates) who will have access to PHI, they must ensure that these subcontractors also comply with HIPAA regulations.
Failure to comply can result in significant penalties, making it essential for both covered entities and their business associates to prioritize HIPAA compliance.
Also read: 13 Best HIPAA Compliance Software
HIPAA: Exceptions and non-covered entities

While HIPAA covers many organizations in the healthcare sector, certain entities are not considered covered entities. These include:
- Employers: Generally, employers are not subject to HIPAA unless they provide health plans. However, they must adhere to other privacy laws regarding employee health information.
- Life Insurers: Insurance companies that offer life insurance products are not covered under HIPAA, as they do not provide healthcare services or health plans.
- Certain educational institutions: Schools and universities that handle student health records may be governed by FERPA (Family Educational Rights and Privacy Act) rather than HIPAA.
The lack of coverage under HIPAA means that these entities are not bound by its privacy and security requirements. However, they still have legal and ethical obligations to protect personal information.
For instance, employers must ensure that employee health data is kept confidential, and educational institutions must safeguard student health records per applicable laws. Understanding these distinctions is crucial for compliance and the proper handling of sensitive information.
Also read: HIPAA Compliance Checklist: Safeguarding Data Privacy Made Easy
Importance of training, policies, and procedures
Training employees on HIPAA regulations is essential to ensure that everyone within the organization understands their responsibilities in safeguarding patient information.
Establishing clear policies and procedures helps to create a culture of compliance and facilitates the proper handling of PHI.
Regular training sessions and updates on HIPAA requirements can mitigate the risk of breaches and non-compliance.
Also read: HIPAA vs HITRUST: A practical comparison for making compliance decisions
Wrapping up
HIPAA provides a crucial framework for protecting patient privacy and ensuring responsible handling of health information. Healthcare professionals and organizations need to prioritize compliance to safeguard patient information and maintain trust within the healthcare system.
Regular training, robust policies, and ongoing risk assessments are key to fostering a culture of compliance. Staying informed about HIPAA regulations is vital for everyone in the healthcare sector.
To enhance your compliance efforts, leverage tools like Scrut, which can streamline your processes and ensure adherence to necessary standards. Get in touch with Scrut today to take proactive steps to prioritize patient privacy, creating a safer and more secure healthcare environment for all.
Frequently Asked Questions
1. What types of entities are considered covered under HIPAA?
Covered entities under HIPAA include health care providers who transmit health information electronically, health plans (such as insurance companies), and health care clearinghouses that process health information.
2. How do business associates relate to HIPAA compliance?
Business associates are individuals or entities that perform functions on behalf of a covered entity that involves the use or disclosure of protected health information (PHI). They are required to comply with HIPAA regulations and have contracts in place with covered entities to ensure PHI protection.
3. Are employers subject to HIPAA regulations?
Employers are generally not considered covered entities under HIPAA unless they provide health plans. However, they must still comply with other privacy laws that protect employee health information.
4. What are the consequences of non-compliance with HIPAA?
Non-compliance with HIPAA can lead to significant penalties, including fines ranging from hundreds to millions of dollars, depending on the severity of the violation, as well as potential civil or criminal charges.
5. How does HIPAA protect patient privacy?
HIPAA establishes national standards for the protection of health information, ensuring that patients’ personal and medical information is kept confidential. It grants patients rights over their health information, including the right to access and request corrections to their records.
Table of contents